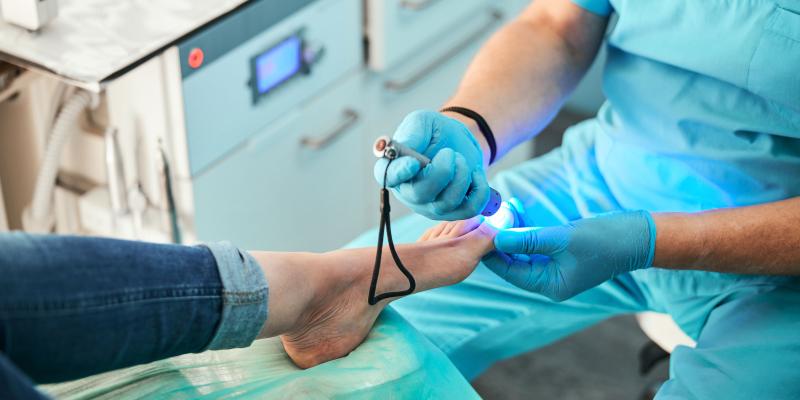
People with diabetes can develop many different foot problems. Even ordinary problems can get worse and lead to serious complications.
Foot problems most often happen when there is nerve damage, also called neuropathy. This can cause tingling, pain (burning or stinging), or weakness in the foot. It can also cause loss of feeling in the foot, so you can injure it and not know it. Poor blood flow or changes in the shape of your feet or toes may also cause problems.
Take good care of your feet and see your doctor right away if you see any signs of foot problems.
Take care of your feet with diabetes
When you have diabetes, caring for your feet is very important in avoiding serious foot complications. Take care of your feet by doing the following:
- Wash your feet thoroughly everyday
- Dry them thoroughly, and don’t forget to dry between your toes
- Moisturize your feet, but avoid moisturizing between your toes
- Keep your toenails trim, and use an emery board to file down sharp edges
- Check your feet for sores, cuts, blisters, corns, or redness daily. Let your doctor know if you find any of these.
- Wear moisture-wicking socks
- Before putting your shoes on, check for sharp objects (i.e. small rocks)
- Wear shoes that fit well and don’t rub your feet
While you’re at it, avoid these:
- Don’t walk around barefoot
- Don’t soak your feet
- Don’t smoke